For many years, endometriosis has been described in a very simple way: “womb lining growing outside the uterus.”
While that explanation is technically related to the condition, it fails to capture the true complexity of endometriosis, and it certainly doesn’t reflect the experience of millions of women living with it.
Endometriosis is increasingly understood as a chronic inflammatory disease that behaves in surprisingly aggressive ways within the body. The condition can implant on organs, invade surrounding tissue, form scar tissue, and trigger ongoing inflammation.
Although endometriosis is not cancer, researchers often note that it shares several biological behaviours with cancer, including the ability of lesions to implant, recruit blood supply, invade nearby tissue, and recur after treatment.
Understanding endometriosis in this way helps explain why symptoms can be severe and why the condition can affect far more than just periods.
What Is Endometriosis?
Endometriosis occurs when tissue similar to the lining of the uterus (endometrium) grows outside the womb.
These cells can attach to structures within the body such as:
- The ovaries
- Fallopian tubes
- The pelvic lining (peritoneum)
- The bladder
- The bowel
- Ligaments supporting the uterus
- Brain, lung, liver, skin, even bone
Unlike normal uterine lining, these cells trigger:
- Local inflammation
- Irritation of surrounding tissue
- Immune system activation
- Scar tissue formation (adhesions)
Over time this can lead to chronic pelvic pain, organ irritation, digestive symptoms, fatigue, and fertility challenges.
Endometriosis affects around 1 in 10 women worldwide, yet diagnosis still takes an average of 7–10 years.
Why Some Experts Compare Endometriosis to Cancer
Endometriosis is not a cancer, but scientists have identified several biological behaviours that resemble cancer-like processes.
These include:
Tissue invasion
Endometriosis lesions can grow into surrounding tissues and beyond, including the bowel, bladder, pelvic nerves, lung, brain and bone.
Angiogenesis
Lesions can stimulate the formation of new blood vessels, allowing them to survive and grow.
Recurrence
Even after surgical removal, endometriosis may return.
Inflammatory environment
The condition creates a persistent inflammatory state within the pelvis.
This does not mean endometriosis becomes cancer, but it does help explain why the disease can behave in ways that are far more complex than simply misplaced uterine lining.
The Four Stages of Endometriosis
Specialists classify endometriosis using a staging system developed by the American Society for Reproductive Medicine (ASRM).
The stage is usually determined during laparoscopy, a keyhole surgery that allows doctors to visualise the pelvis.
Endometriosis is divided into four stages:
- Stage I – Minimal
- Stage II – Mild
- Stage III – Moderate
- Stage IV – Severe
The classification is based on:
- Number of lesions
- Depth of invasion
- Presence of scar tissue
- Ovarian cysts (endometriomas)
However, the stage does not reliably predict how severe symptoms will be.
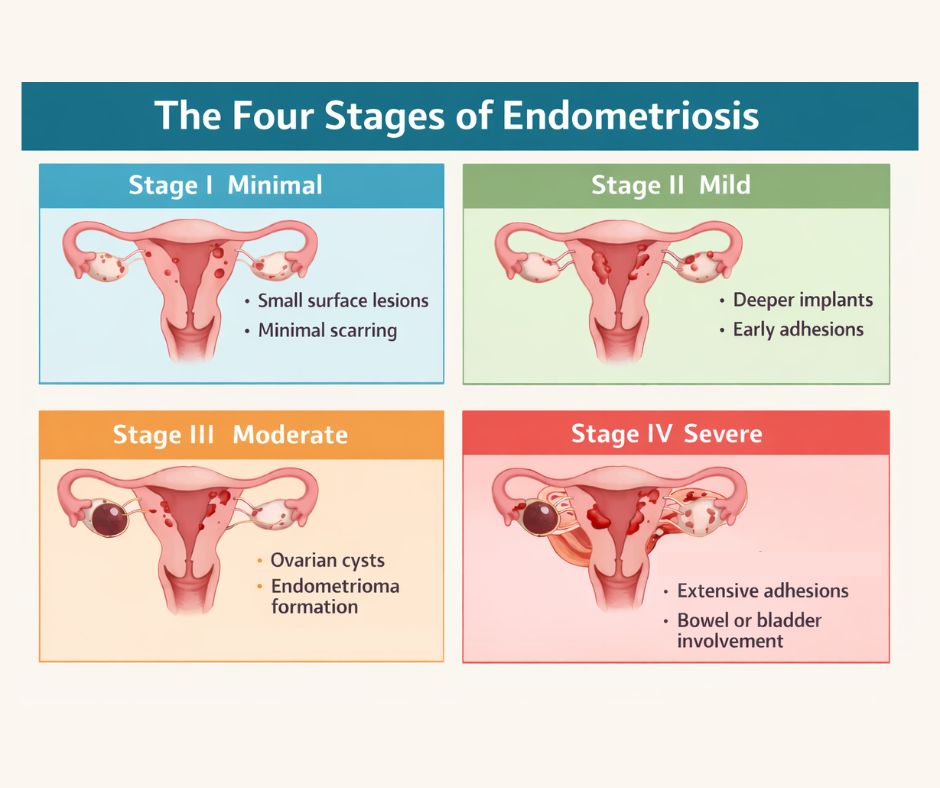
Stage I Endometriosis (Minimal)
Stage I disease involves small superficial lesions on the pelvic lining.
There are typically:
- Few implants
- Surface-level lesions
- Minimal scar tissue
Despite appearing “minimal,” inflammation around these lesions can still trigger significant symptoms.
Many women with Stage I disease experience severe period pain, pelvic discomfort, or fatigue.
Stage II Endometriosis (Mild)
Stage II disease involves a greater number of lesions, some of which may grow slightly deeper into pelvic tissues.
At this stage:
- Lesions may be deeper
- Early scar tissue may begin to form
- Pain may start occurring outside of menstruation
Symptoms may include worsening period pain, pelvic pain between cycles, pain during sex, and discomfort with bowel movements during periods.
Stage III Endometriosis (Moderate)
Stage III disease typically includes:
- Multiple deep implants
- Adhesions (scar tissue)
- Small ovarian cysts called endometriomas
Scar tissue can cause organs within the pelvis to stick together, which may contribute to pain and fertility challenges.
Women at this stage may experience chronic pelvic pain, severe menstrual cramps, painful intercourse, and digestive symptoms during menstruation.
Stage IV Endometriosis (Severe)
Stage IV is the most advanced stage of endometriosis.
It often includes:
- Large ovarian endometriomas
- Extensive adhesions
- Deep infiltrating lesions
- Possible involvement of the bowel or bladder
In some cases, scar tissue can distort pelvic anatomy.
Symptoms may include severe pelvic pain, bowel or bladder symptoms during menstruation, painful sex, and fertility difficulties.
However, some women with Stage IV disease may still have relatively mild symptoms.
Why Symptoms Don’t Always Match the Stage
One of the most confusing aspects of endometriosis is that pain severity does not always match the stage of disease.
Several factors influence symptoms, including:
Location of lesions
Small implants near pelvic nerves can cause severe pain.
Inflammation
Endometriosis releases inflammatory chemicals that amplify pain signals.
Nerve sensitisation
Chronic inflammation can make the nervous system more sensitive to pain.
Individual immune response
Different people respond to inflammation differently.
For this reason, treatment decisions are usually based on symptoms and quality of life rather than stage alone.
How Endometriosis Is Diagnosed
Diagnosis usually begins with a discussion of symptoms and medical history.
Investigations may include:
- Pelvic ultrasound (in experienced hands)
- MRI scanning with contrast looking specifically for endometriosis (and reviewed by experienced specialists)
- Diagnostic laparoscopy (in experienced hands)
At present, laparoscopy remains the only definitive way to confirm endometriosis, although there are now less invasive diagnostic tools such as the Ziwig Endo Test, but it isn’t yet in widespread use.
Treatment Options for Endometriosis
Management depends on symptoms, fertility plans, and individual circumstances.
Treatment approaches may include:
Hormonal treatments
Hormonal therapies aim to reduce stimulation of endometriosis tissue.
Examples include:
- Combined contraceptive pill
- Progestogen treatments e.g. slynd
- Hormonal intrauterine systems
- GnRH analogues in selected cases
Pain management
Anti-inflammatory medications and multidisciplinary pain approaches can help manage symptoms.
Surgery
Laparoscopic surgery may be used to remove lesions, endometriomas, and scar tissue.
Complex cases may require treatment in specialist endometriosis centres.
Frequently Asked Questions About Endometriosis
What are the early signs of endometriosis?
Early symptoms often include painful periods that worsen over time, pelvic pain outside menstruation, pain during sex, painful bowel movements during periods, and fatigue.
Some women also experience bloating, sometimes called “endo belly.”
Does the stage of endometriosis affect pain levels?
No. Pain severity does not reliably correlate with the stage of disease.
Some women with minimal disease experience severe pain, while others with advanced disease have relatively mild symptoms.
Can endometriosis affect fertility?
Endometriosis can affect fertility by causing inflammation, scar tissue, and distortion of pelvic anatomy.
However, many women with endometriosis are still able to conceive naturally.
Can endometriosis return after surgery?
Yes. Endometriosis can recur after surgery, with recurrence rates estimated at 20–40% within five years.
Because it is a chronic condition, long-term management is often required.
Resources and Charities for Endometriosis Support
Endometriosis UK
https://www.endometriosis-uk.org
The UK’s leading charity supporting people with endometriosis. They provide education, support groups, and a national helpline.
British Society for Gynaecological Endoscopy
https://www.bsge.org.uk/endometriosis-centres
Provides information about accredited specialist endometriosis centres in the UK.
Wellbeing of Women
https://www.wellbeingofwomen.org.uk
A charity funding research into female reproductive health, including endometriosis.
Fertility Network UK
https://fertilitynetworkuk.org
Provides information and support for individuals experiencing fertility difficulties.
Final Thoughts
Endometriosis is far more than “bad periods.” It is a complex inflammatory disease that can affect multiple organs, disrupt daily life, and take years to diagnose.
Recognising the condition early, seeking appropriate medical support, and accessing specialist care can make a significant difference to long-term health and quality of life.
We can offer support with this through our endometriosis package. You don’t need to suffer for multiple years before reaching the diagnosis.
